Diabetic Foot Care
What is diabetic foot?
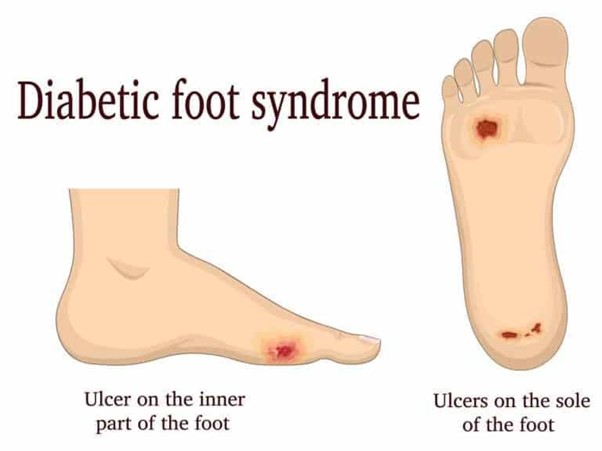
Diabetics are at increased risk of developing foot wounds and is the most common cause of foot ulcers, infection, and amputation. Approximately 25% of diabetics will develop a foot wound in their lifetime.
Many factors can lead to diabetic foot wounds: diminished foot sensation, altered foot mechanics, decreased sweating , structural changes in the foot, and peripheral arterial disease (PAD). Diabetics have an increased prevalence of atherosclerosis (the main cause of PAD) which narrows the blood vessels of the leg and within the foot.
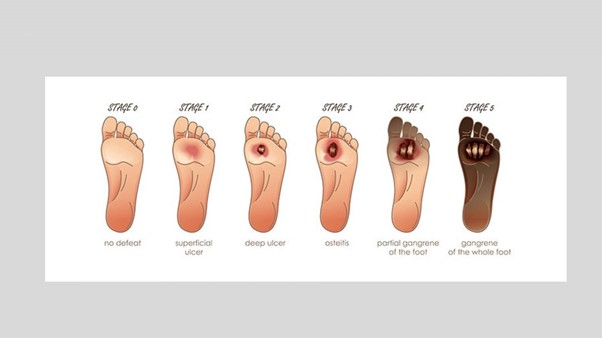
One very important feature of the diabetic foot is identifying predisposing factors prior to onset of complications. Diabetics should inspect their feet and shoes regularly searching for signs of skin irritation, abnormal wear and foreign materials. Any wound needs close attention.
Treatment options
Apart from non-surgical treatment, surgery for a complicated diabetic foot wound may be needed to address the foot wound itself, correct the underlying cause for the wound forming the the first place, and improve the foot environment to maximize the chance of healing. Infected dead tissue around a wound may need to be removed. If the wound is large or the infection is severe, amputation may be necessary. To improve the circulation to the foot, a bypass operation may be recommended.
To open blocked blood vessels and improve the circulation to the foot, sometimes and endovascular treatment option is appropriate. Endovascular techniques involve guiding balloons through blood vessels which are inflated to open blockages. Sometimes a stent is needed to keep a treated blood vessel open. Endovascular treatments are less invasive, but may not be suitable for all types of blocked blood vessels.
